Top 10 Proven Stem Cell Treatments (2022)
Trying to keep up with the latest stem cell therapy evidence? There are more than 240,000 scientific publications published on "stem cell' on the National Library of Medicine (PubMed). As of July 2022, more than 8,000 studies have been launched to investigate the potential of stem cell therapy under the U.S. Clinical Trial Registry. There's a lot to read and catch up to. How do we keep up with all these stem cell therapy evidence?
www.onedaymd.com
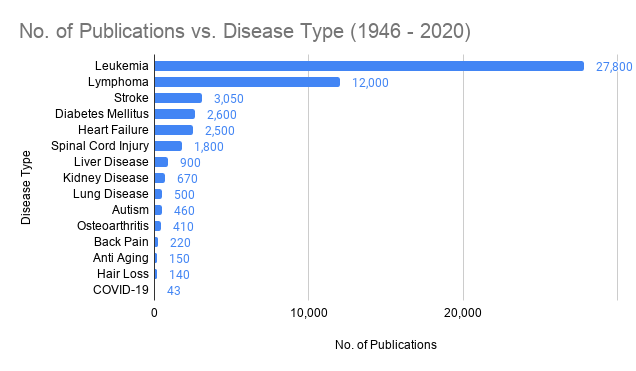 |
| Stem Cell Research Summary |
Stem cell therapy has recently gained popularity as a promising treatment option for conditions where the current medical treatment protocols have been exhausted. However, there is also a lot of confusion due to the overwhelming mixing of credible scientific information and marketing hypes available on the internet.
We do get the following questions very frequently: Does it really work? Is it safe? Is it a scam? Is there any scientific evidence? How do you get the stem cells?
If you are new to stem cells, check out stem cell basics.
Due to the fast-changing pace of research and technology, new evidence accumulates rapidly and clinical guidelines need to be periodically updated.
We have compiled and summarised essential information below in layman's terms so that you can understand and make a better informed decision.
This article contains information and links to list of stem cell therapy and research in various categories. This list is a work-in-progress list as new evidence might be added from time to time.
In this Article:
- Leukemia
- Lymphoma
- Stroke
- Osteoarthritis
- Diabetes
- Spinal Cord Injury
- Autoimmune Diseases
- Heart Diseases
- Autism
- Anti-Aging
STEM CELL THERAPY EVIDENCE AND RESEARCH BY CATEGORY
Here, we have listed and compiled all significant scientific publications related to stem cell therapy. The list was complied by running various searches on PubMed. Each study is hyperlinked to the abstract in the U.S. National Library of Medicine or the full text article to make it easier for healthcare providers or scientists to access more details. The list was complied by running various searches on PubMed.
In order to make it consumer friendly, we have tried to summarise the studies and minimise the technical jargons.
Below are 10 of the most popular stem cell treatments right now. Here is the list by category.
In order to make it consumer friendly, we have tried to summarise the studies and minimise the technical jargons.
Below are 10 of the most popular stem cell treatments right now. Here is the list by category.
1. Leukemia
Leukemia is another form of cancer that affects the lymphatic system as well as bone marrow. Leukemia cells are cancerous, affecting the immune system and causing an array of unpleasant symptoms, then eventually leading to death without treatment. It is the most common childhood cancer, but it affects adults of a range of ages as well.There are more than 30,000 publications related to the use of stem cells in leukemia. As of July 2022, there are more than 1,000 studies that have been launched to investigate the benefits of stem cell therapy and leukemia. You can review the status and details of these trials on clinicaltrials.gov.
Stem cell therapy poses significant hope, however. Much like with non-Hodgkin’s lymphoma, the treatment involves first killing off leukemia cells with high doses of chemotherapy and sometimes radiation as well. After the majority of cancer cells are defeated, the patient receives an infusion of stem cells to help the body repopulate, so that it can make normal blood cells once again.
This treatment, like the one for non-Hodgkin’s lymphoma, is typically only available to patients who have relapsed. That means their cancer went into remission from standard treatments, then returned months or years later. Good news, though: with a stem cell treatment within the first remission, the survival rate at 5 years is 30-50 percent. If the patient has not experienced a relapse within 2 years of the stem cell transplant, they have a good chance of surviving for many years.
2. Non-Hodgkin’s Lymphoma
Non-Hodgkin’s lymphoma is a type of cancer that arises in the lymphatic system, which is responsible for fighting disease and toxins in the body. White blood cells, also known as lymphocytes, give rise to cancer cells, which then pervade the body. Without treatment, the condition is almost universally fatal.
Chemotherapy is an extremely effective tool against this disease. The problem is, high doses of chemotherapy often kill off bone marrow, in which new blood cells get made. In so doing, the chemotherapy kills cancer but also kills the patient, who now has no source of blood cells.
Stem cell treatment, however, helps mitigate this risk substantially by giving the patient an infusion of new cells following those necessarily high doses of chemotherapy. The patient first receives the chemo, then the stem cell infusion to help them repopulate their blood cell counts. Many patients show great promise of living long and healthy lives following the treatment.
Chemotherapy is an extremely effective tool against this disease. The problem is, high doses of chemotherapy often kill off bone marrow, in which new blood cells get made. In so doing, the chemotherapy kills cancer but also kills the patient, who now has no source of blood cells.
Stem cell treatment, however, helps mitigate this risk substantially by giving the patient an infusion of new cells following those necessarily high doses of chemotherapy. The patient first receives the chemo, then the stem cell infusion to help them repopulate their blood cell counts. Many patients show great promise of living long and healthy lives following the treatment.
There are more than 14,000 publications related to the use of stem cells in lymphoma. As of May 2022, there are more than 900 studies that have been launched to investigate the benefits of stem cell therapy and lymphoma. You can review the status and details of these trials on clinicaltrials.gov.
3. Stem Cell Therapy for Stroke
There are more than 3,000 publications related to the use of stem cells and stroke. As of May 2022, there are more than 60 studies that have been launched to investigate the benefits of stem cell therapy and stroke. You can review the status and details of these trials on clinicaltrials.gov.Stroke constitutes the second leading cause of death worldwide. Stem cell therapy that has been developed over the past several decades represents a promising alternative or supplemental strategy; notably, this approach has already reached the translational stage, with therapeutic results in humans having been discussed in various publications.
In this review (published in Nature), the authors examined the clinical research trends related to stem cell therapy products in the stroke space based on information obtained from the ClinicalTrials.gov website and International Clinical Trials Research Platform (ICTRP) portal site.
Within hours of the stem cell treatment, she was able to move her arms and legs – whereas before she had suffered almost complete immobilization. She and her doctors also noticed rapid improvements in her speech – again, within only a few hours. Other patients noticed astonishing improvements as well, the only side effects coming in the form of “passing headaches.”
4. Stem Cell Therapy for Osteoarthritis
Osteoarthritis is a degenerative condition affecting the joints. Over time, the cartilage that protects joints, preventing the rubbing of one bone on another, breaks down. Eventually, this can lead to the deterioration of the underlying bone as well, causing aching, stiffness, and eventual immobility in many cases. The condition commonly affects the hips, knees, and thumbs, though it can also strike elbows, wrists, ankles, and fingers.
Some doctors and media channels argue that there is very little evidence to support the use of stem cells to treat orthopaedic conditions. However, there are more than 1,700 publications related to the use of stem cells in treating orthopaedic conditions. There are currently more than 120 studies on stem cell treatment for osteoarthritis under the U.S. Clinical Trial Registry.
Several other comparative studies have demonstrated good evidence in the treatment of osteoarthritis. However, there are several approaches and cell lines used. More well-designed and randomised controlled trials are needed to evaluate the best approach and universal consensus. As studies continue, the methods, forms and combinations of stem cell preparations are improving, and outcomes are expected to improve as well.
Stem cell procedure is offered in many clinics within and outside the United States and typically uses adipose cells as the stem cell source. Physicians extract these cells from fat tissue, separate out the stem cells from the rest, then prepare a solution containing growth factors and other ingredients necessary to tell stem cells how to develop in the new site. Once it’s prepared, doctors inject it into the affected site, such as a knee joint.
Regenexx is a U.S. company specializing in orthopedic applications of stem cells that was founded by Dr. Chris Centeno. Dr. Centeno is an expert in the clinical use of mesenchymal stem cells (MSCs) within orthopedic applications. His Regenexx clinic in Denver, Colorado, draws patients from all over the U.S. who are seeking innovative, non-surgical treatments for osteoarthritis, as well as a wide range of other orthopedic applications.
As the visionary behind the revolutionary Regenexx® technology, he pioneered a procedure that involves extracting a small bone marrow sample through a needle and a blood draw from a vein in your arm. These samples are then processed in a laboratory and the stem cells it contains are injected into the area needing repair. The goal is to deliver large numbers of stem cells to the injured area.
Stem cell procedure is offered in many clinics within and outside the United States and typically uses adipose cells as the stem cell source. Physicians extract these cells from fat tissue, separate out the stem cells from the rest, then prepare a solution containing growth factors and other ingredients necessary to tell stem cells how to develop in the new site. Once it’s prepared, doctors inject it into the affected site, such as a knee joint.
Regenexx is a U.S. company specializing in orthopedic applications of stem cells that was founded by Dr. Chris Centeno. Dr. Centeno is an expert in the clinical use of mesenchymal stem cells (MSCs) within orthopedic applications. His Regenexx clinic in Denver, Colorado, draws patients from all over the U.S. who are seeking innovative, non-surgical treatments for osteoarthritis, as well as a wide range of other orthopedic applications.
As the visionary behind the revolutionary Regenexx® technology, he pioneered a procedure that involves extracting a small bone marrow sample through a needle and a blood draw from a vein in your arm. These samples are then processed in a laboratory and the stem cells it contains are injected into the area needing repair. The goal is to deliver large numbers of stem cells to the injured area.
Regenexx, the largest provider of stem cell therapy for orthopaedic conditions in the United States alone, have treated 30,000 patients with stem cell therapy for various joint conditions including knee pain.
www.onedaymd.com
There are more than 3,000 publications related to the use of stem cells in diabetes mellitus. As of May 2022, there are more than 130 studies that have been launched to investigate the benefits of stem cell therapy and diabetes mellitus. You can review the status and details of these trials on clinicaltrials.gov.
Many people are very interested in the possibility of stem cells to treat diabetes. Both Type I and Type II diabetes have devastating effects on the health of millions, and stem cells may help to ameliorate those conditions.
Type I and Type II diabetes affect the body in different ways. Type I diabetes is genetic, and results from the pancreas failing to produce insulin, or producing too little of it. Insulin is what tells the body to remove glucose from the bloodstream and let it into cells, so they can use it for energy. Most likely this is due to an immune system disorder in which the body attacks its own islets, the pancreatic cells responsible for manufacturing insulin. In this case, stem cells may provide the same immune system-modulating effect as they do for other autoimmune diseases.
Type II diabetes is when the body becomes resistant to insulin. The pancreas may still make it, but the patient’s body does not sense it – it is “insulin resistant,” which means the release of insulin in the bloodstream still does not result in cells taking up glucose. It remains in the bloodstream, causing dangerous hyperglycemia just as it does in the case of Type I.
The second condition may also respond to stem cell treatment, which can help moderate pancreatic productive of insulin as well as helping the body respond to it more effectively. Multiple clinical trials assessing the validity of stem cells for both diseases are underway, and many eagerly await their results.
Type I and Type II diabetes affect the body in different ways. Type I diabetes is genetic, and results from the pancreas failing to produce insulin, or producing too little of it. Insulin is what tells the body to remove glucose from the bloodstream and let it into cells, so they can use it for energy. Most likely this is due to an immune system disorder in which the body attacks its own islets, the pancreatic cells responsible for manufacturing insulin. In this case, stem cells may provide the same immune system-modulating effect as they do for other autoimmune diseases.
Type II diabetes is when the body becomes resistant to insulin. The pancreas may still make it, but the patient’s body does not sense it – it is “insulin resistant,” which means the release of insulin in the bloodstream still does not result in cells taking up glucose. It remains in the bloodstream, causing dangerous hyperglycemia just as it does in the case of Type I.
The second condition may also respond to stem cell treatment, which can help moderate pancreatic productive of insulin as well as helping the body respond to it more effectively. Multiple clinical trials assessing the validity of stem cells for both diseases are underway, and many eagerly await their results.
Currently, two approaches are being used in research, using stem cells as beta-cell producing factories or as a beta cell repair catalyst. Both methods have the same goal which is to return the insulin to normal levels. Diabetes Research Institute (DRI) are running clinical trials and have a number of patients that are living insulin free after receiving a transplant of donor islet cells.
There are many ongoing efforts to understand how stem cell therapy is able to help people with diabetes. One of the main centres is the California Institute of Regenerative Medicine, where you can view the areas of research being conducted specifically to understand diabetes.
A review, published in the Progress in Stem Cell journal in 2019 suggested a combination of antioxidants, growth factors or hormones along with MSCs (mesenchymal stem cells) in optimal combinations and concentrations for the treatment of diabetic nephropathy.
6. Stem Cell Therapy for Spinal Cord Injury
One of the most traumatic injuries to the human body is severing of the spinal cord. Depending on where the injury occurs, the patient may never walk or even move their arms again. For most of human history, such a traumatic injury was completely irreparable. In recent years, neurosurgery has given people back some of their function in cases like these, but outcomes are still all too often disappointing.
Stem cells provide serious hope for the future. Instead of trying to repair damaged nerves, stem cells offer the ability to replace them. By injecting stem cells to the site of the injury, the spinal column can repair itself, accessing all the ingredients it needs for the specialized job.
In combination with growth factors and hormones, stem cells are capable of traveling to the site of the injury “assessing” what needs rebuilding and stepping in to do the job for doctors. This limits the number of modifications needed from the outside and leaves the healing to the body.
While the mechanisms aren’t yet clear, it seems that hormones such as growth factors – in addition to the location in the body – can provide signposts to stem cells telling them what kinds of tissues are needed. Then the stem cells transform into them, integrate with the damaged tissue and repair it.
One of the most traumatic injuries to the human body is severing of the spinal cord. Depending on where the injury occurs, the patient may never walk or even move their arms again. For most of human history, such a traumatic injury was completely irreparable. In recent years, neurosurgery has given people back some of their function in cases like these, but outcomes are still all too often disappointing.
Stem cells provide serious hope for the future. Instead of trying to repair damaged nerves, stem cells offer the ability to replace them. By injecting stem cells to the site of the injury, the spinal column can repair itself, accessing all the ingredients it needs for the specialized job.
In combination with growth factors and hormones, stem cells are capable of traveling to the site of the injury “assessing” what needs rebuilding and stepping in to do the job for doctors. This limits the number of modifications needed from the outside and leaves the healing to the body.
While the mechanisms aren’t yet clear, it seems that hormones such as growth factors – in addition to the location in the body – can provide signposts to stem cells telling them what kinds of tissues are needed. Then the stem cells transform into them, integrate with the damaged tissue and repair it.
There are more than 2,000 scientific publications published related to "stem cell" and "spinal cord injury" on the National Library of Medicine.
As of May 2022, more than 60 studies have been launched to investigate the potential of stem cell therapy for spinal cord injuries under the U.S. Clinical Trial Registry.
As of May 2022, more than 60 studies have been launched to investigate the potential of stem cell therapy for spinal cord injuries under the U.S. Clinical Trial Registry.
Related: Stem Cells and Spinal Cord Injury: Can Stem Cells Help Spinal Cord Injury?
7. Autoimmune Diseases
A huge range of autoimmune conditions exists, such as diabetes, rheumatoid arthritis, multiple sclerosis, lupus, Addison’s disease, Grave’s disease, and more.These conditions all share the characteristic of the body’s immune system reacting to normal substances in the body as though they were pathogenic. That means instead of letting the body function normally, the immune system will attack tissues and substances, creating ongoing sickness and in many cases, eventually death.
Stem cell therapy has two possible benefits in the case of autoimmune diseases. For one thing, it can help repair and regenerative tissues damaged in an autoimmune attack. Stem cells can help them repair nerves, skin, blood, organs, and more. This helps the patient regain their health and fight the degenerative nature of such diseases.
Second, stem cells can actually modulate the immune system so that it no longer attacks the body so viciously – or at all. Research demonstrates that stem cells can minimize the pathological effects of the immune system, making it so the body no longer attacks itself – all while preserving its ability to attack foreign substances and real pathogens.
There are more than 900 scientific publications published related to "stem cell" and "autoimmune disease" on the National Library of Medicine. As of May 2022, more than 200 studies have been launched to investigate the potential of stem cell therapy for autoimmune diseases under the U.S. Clinical Trial Registry.
8. Heart Diseases and Heart Failure
Heart disease is still the No. 1 killer in the United States (although by some estimates cancer will soon or has already surpassed it). For obvious reasons, stem cells seem like a strong possibility for repairing heart tissue and helping to overcome the intermediate symptoms that eventually lead to heart disease or cardiac arrest.As is the case with most of these therapies, the biggest benefit of stem cell treatment for heart disease is its ability to replace damaged or dead cells without the need for invasive surgery or transplants. An injection of stem cells can give the body the ingredients it needs to grow the specialized cells on site, ideally without having to put the patient under or open them up. The exact mechanisms of this procedure are not as yet clear, however.
On 16 May, 2018, Nature News reported that Japan’s health ministry gave doctors at Osaka University permission to take sheets of tissue derived from stem cells and use them to treat diseased human hearts. From preclinical studies in pigs, it appears that thin sheets of cell grafts grown from induced pluripotent stem cells can improve heart function. While the treatment approved by Japan’s health ministry will only be tested in three patients, a follow-up trial could enroll ten or more patients.
There are more than 1,500 scientific publications published related to "stem cell" and "spinal cord injury" on the National Library of Medicine. As of May 2022, more than 200 studies have been launched to investigate the potential of stem cell therapy for spinal cord injuries under the U.S. Clinical Trial Registry.
9. Stem Cell Therapy for Autism
Stem cell therapy for autism is an ongoing topic of research and is considered experimental by the medical community. Parents can find fee-for-service clinics that advertise stem cell therapy for autism, but most of these clinics are operating without FDA approval, and each clinic promotes their own approach, which creates a lot of confusion among parents about how to compare their treatment options.
There are more than 600 publications related to the use of stem cells and autism. As of May 2022, more than 20 studies have been launched to investigate the potential of stem cell therapy for autism under the U.S. Clinical Trial Registry. You can search the database to look for more details of the clinical trials including the countries and centres that are conducting them.
Stem cell therapy for anti aging is an ongoing topic of research and is considered experimental by the medical community. Is there any evidence that stem cell therapy for anti aging is effective and safe?
There are more than 200 publications related to the use of stem cells and anti-aging. As of May 2022, 3 studies were found for 'stem cell and anti-aging' under the U.S. Clinical Trial Registry.
www.AestheticsAdvisor.com
Despite the fact that there are many published studies on stem cell therapy for anti-aging, major media has been slow to report the findings.
Journal of Gerontology - The results of 2 clinical studies, published in The Journals of Gerontology, showed how a type of adult stem cell called mesenchymal stem cells (MSCs) could reverse the effects of aging.
The first trial involved 15 frail patients, each received single MSC infusion of stem cells collected from adult bone marrow donors aged between 20 and 45 years old. The patients exhibited improved overall quality of life and fitness, as well as diminished tumor necrosis factor levels. The second trial was a double-blind, randomized study involving a placebo group. Aside from noting no adverse effects, the research team found the improvements to be “remarkable.”
We have compiled other related published studies below.
Yu Y. Application of Stem Cell Technology in Antiaging and Aging-Related Diseases. Adv Exp Med Biol. 2018;1086:255-265
Ivonne Hernandez Schulman, Wayne Balkan and Joshua M. Hare. Mesenchymal Stem Cell Therapy for Aging Frailty. Front Nutr. 2018; 5: 108.
Juan Antonio Fafián-Labora, Miriam Morente-López, and María C Arufe. Effect of aging on behaviour of mesenchymal stem cells. World J Stem Cells. 2019 Jun 26; 11(6): 337–346.
www.AestheticsAdvisor.com
Despite the fact that there are many published studies on stem cell therapy for anti-aging, major media has been slow to report the findings.
Journal of Gerontology - The results of 2 clinical studies, published in The Journals of Gerontology, showed how a type of adult stem cell called mesenchymal stem cells (MSCs) could reverse the effects of aging.
The first trial involved 15 frail patients, each received single MSC infusion of stem cells collected from adult bone marrow donors aged between 20 and 45 years old. The patients exhibited improved overall quality of life and fitness, as well as diminished tumor necrosis factor levels. The second trial was a double-blind, randomized study involving a placebo group. Aside from noting no adverse effects, the research team found the improvements to be “remarkable.”
We have compiled other related published studies below.
Yu Y. Application of Stem Cell Technology in Antiaging and Aging-Related Diseases. Adv Exp Med Biol. 2018;1086:255-265
Ivonne Hernandez Schulman, Wayne Balkan and Joshua M. Hare. Mesenchymal Stem Cell Therapy for Aging Frailty. Front Nutr. 2018; 5: 108.
Juan Antonio Fafián-Labora, Miriam Morente-López, and María C Arufe. Effect of aging on behaviour of mesenchymal stem cells. World J Stem Cells. 2019 Jun 26; 11(6): 337–346.
www.AestheticsAdvisor.c
Stem Cell Therapy for Other Indications
The public may search a database of NIH-sponsored clinical trials at www.clinicaltrials.gov. Enter the search terms of interest (e.g., Parkinson's Disease and stem cells) to search for applicable clinical trials.
The public may search a database of NIH-sponsored clinical trials at www.clinicaltrials.gov. Enter the search terms of interest (e.g., Parkinson's Disease and stem cells) to search for applicable clinical trials.
Conclusion
If there are any new major stem cell related evidence that we’ve missed, please let us know in the comments and we’ll add them to the post! Thank you in advance.


Comments
Post a Comment